Athlete's Foot
Is tinea causing that itching between your toes?
How can you effectively treat tinea?
Athlete’s foot (also known as tinea pedis) is a very common condition that will affect most people sometime during their life. Characterised by intense itching between the toes, and a red rash, this fungal infection can get out of control if you don’t seek treatment. We are highly experienced in treating athlete’s foot and see many cases in our podiatry clinic.
Find out more about athlete’s foot, including how you can prevent it, and how we can help treat it.
What is tinea pedis?
Tinea pedis is a common foot infection caused by fungi called dermatophytes, that live on the dead tissues of your skin, hair and nails. The infection usually begins between the toes but can spread to other parts of your feet, and your hands — especially if you scratch the affected area.
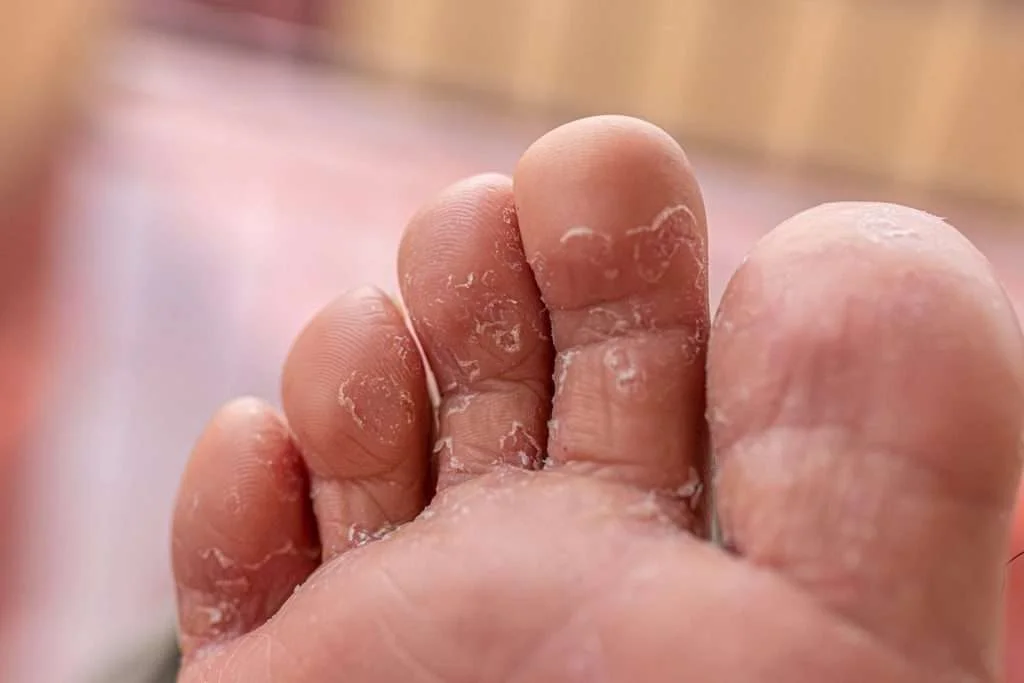
Why is it called athlete’s foot?
Tinea pedis is commonly called athlete’s foot because dermatophytes are especially common in warm, moist environments and therefore tend to affect people with damp or sweaty feet — like athletes. However, anyone can get this infection.
Signs and symptoms of athlete's foot?
Athlete’s foot has a number of signs and symptoms including:
- intense itching, especially between the toes
- itching that is worse when you remove your shoes and socks
- blisters on your feet that are itchy
- red, scaly rash
- peeling, flaking or cracking of the skin, especially between your toes

What causes tinea on your feet?
Dermatophytes are fungi that usually live on the skin, hair and nails — the same fungi that cause ringworm and jock itch. When these environments get warm and moist, they grow out of control and cause the symptoms of athlete’s foot.
You can also catch the fungus through direct contact with an infected person, or by touching surfaces such as floors, showers or even towels that have been contaminated by an infectious person.
Who is at risk of developing athlete’s foot?
Anyone can develop athlete’s foot, but it’s more common in people who:

have damp or wet feet for long periods of time

often have sweaty feet.

share socks or towels with other people

wear tight, closed-in shoes

walk barefoot in communal areas where the infection can spread such as showers, locker rooms and swimming pools
Complications of athlete’s foot
If not effectively treated, athlete’s foot infection can spread to other parts of your body which include:
- hands — particularly if you scratch and pick at the infected part of your feet
- nails — toenails can also become infected causing fungal toenails which can be more resistant to treatment
- groin — as the fungi that cause tinea also cause jock itch, it’s common for the infection to be transferred to your groin area via towel or hand.
If the skin becomes cracked or split, it’s possible for bacteria to enter and cause a bacterial infection called cellulitis. However, this is more common in people with diabetes, weakened immune systems, and the elderly.
Treatment for tinea
Effectively treating tinea can take several weeks or even months, and the infection can return if the warm, moist conditions persist. Long-term treatment usually requires a change in how you look after your feet, and the footwear you choose.
home treatment
The first line of treatment for tinea is usually an over-the-counter (OTC) antifungal preparation available through your pharmacy. These are usually in the form of powders, creams or sprays.
Avoid scratching, tearing or scraping off flaking skin as this can spread the infection further. You will also need to practice good hygiene during treatment. This means:

washing and drying your feet thoroughly (especially between the toes) every morning and evening

changing your socks or stockings daily

swapping your cotton or bamboo socks for moisture-wicking socks that will help keep your feet drier

avoiding wearing the same shoes day after day — give them a chance to air out

use an antifungal cream on your feet each day

giving your feet ‘air time’ by going barefoot or wearing thongs or sandals if possible.
In order to prevent the infection from recurring, continue treatment for up to two weeks after the infection has cleared.
Podiatry treatment
Most people get a bout of athlete’s foot sometime during their life which clears up with home treatments. However, sometimes it can recur or not respond to OTC treatments. If this is the case, we recommend you come and see us. You should also make an appointment if:
- your cracked skin is bleeding
- you have white, soggy skin between your toes
- there is an unpleasant smell associated with your tinea
- you have painful blisters that are oozing
- you are experiencing pain in the affected area
- your nails are affected
Our friendly podiatrists can help diagnose your athlete’s foot, recommend the best treatment, and provide advice on how to prevent the infection from recurring. We can also provide assistance with the most stubborn of tinea infections, including nail infections.
How to prevent athlete’s foot
The key to preventing athlete’s foot is focusing on good hygiene. You should:

change your socks regularly, especially if they get sweaty playing sport

wear light, well-ventilated shoes as often as possible

choose socks that wick-away moisture.

avoid wearing the same shoes each day to give them time to dry out between wears

avoid going barefoot in communal showers, swimming pools or locker rooms

use an antifungal cream on your feet each day

avoid sharing shoes and socks

keep your feet dry, especially between your toes, by airing them out and thoroughly drying between them after bathing, showering or swimming
Frequently asked questions
Topical antifungal treatments for athlete’s foot have been deemed to pose a negligible risk to a breast-feeding baby. That said if it is a minor infection, we suggest that patients might use natural therapies such as daily apple cider vinegar soak, maintain dry feet and use alcohol wipes between toes after the shower.
Research is limited regarding use of topical antifungal medication during pregnancy. Treatment plans should be based on the severity of infection – your consulting Podiatrist might be able to suggest some home remedies that can clear the infection without need for medication.
Yes. There are a multitude of treatment options that can be matched to each person and the severity of infection. Ask your treating Podiatrist which treatments best suits your individual case.
Yes. Depending on the location, skin type, immune system and infecting organism Athlete’s Foot can cause blisters on the feet. During the consultation your Podiatrist can provide information on the management of these blisters and also the best treatment plan to resolve the underlying infection.
Fungal infection of the hands is called Tinea Manuum, it is far less common than Athlete’s foot. We suggest patient avoid touching their feet whilst suffering from Athlete’s foot to avoid cross infection.
Athlete’s Foot if untreated can become more severe and potentially spread. It is believed that chronic tinea can be a major cause of fungal toenail infections. It is best to commence treatment as soon as you notice signs or symptoms of infection.
The best way to treat Athlete’s foot is prevention. Keep your feet dry, change socks regularly if you suffer from sweaty feet, avoid walking barefoot in common areas like the public swimming pools or bathrooms. Treatment should be based on severity; when necessary natural treatments such as apple cider vinegar, tea tree oil, hydrogen peroxide, salt bath or potassium permanganate foot soaks can be used however these will not always be effective. It is recommended you speak to a Podiatrist prior to commencing any treatment.
Yes. Oral Lamisil is one of the most effective way of clearing fungal skin infection – it is however reserved for recurrent infections that do not resolve with traditional topical or photodynamic treatment options.
Yes. It is advised that members in the same household wear thongs in bathrooms or hard floors. Cross infection can also be reduced by keeping feet dry, changing socks regularly and regularly cleaning bathroom surfaces with bleach.
Yes. Fungal infections can occur at any age. Many topical antifungals are not recommended for use on children < 12 years old. Consult your Podiatrist for the best treatment options for infants and young children.
Yes. There is no issue with swimming however we don’t recommend you get the feet wet if the infection has caused splits or fissures. Breaks in the skin does increase risk of developing a bacterial infection. If swimming at public swimming pools we recommend you wear thongs to protect other patrons.
No. It is best to see your Podiatrist first and clear the athlete’s foot infection prior to resuming regular pedicures.
There are a number of over-the-counter topical treatments that can be purchased from your local pharmacy. For best results it is best to see a Podiatrist to confirm diagnosis and to tailor a treatment plan that best suits your needs.
For minor Athlete’s Foot infection you can try use of Apple cider vinegar at a ratio of 1 part apple cider vinegar :2 parts water. Soak for 15 minutes twice a day for 2 weeks.
- Dry skin: Tips for managing. American Academy of Dermatology. https://www.aad.org/public/diseases/dry-sweaty-skin/dry-skin#overview. Accessed Feb. 18, 2019.
- Kermott CA, et al., eds. In Mayo Clinic Book of Home Remedies. 2nd ed. New York, N.Y.: Time Inc. Books; 2017.
- Litin SC, et al., eds. Skin, hair and nails. In: Family Health Book. 5th ed. Rochester, Minn.: Mayo Foundation for Medical Education and Research; 2018.
- Gibson LE (expert opinion). Mayo Clinic, Rochester, Minn. Feb. 18, 2019.
- Pawar M. The title of the paper: Treatment of painful and deep fissures of heel with topical timolol. J Am Acad Dermatol. 2020 May 29:S0190-9622(20)30975-0. doi: 10.1016/j.jaad.2020.05.100. Epub ahead of print. PMID: 32479981.
- IGNATOFF WB. Heel fissures and their management. J Natl Assoc Chirop. 1952 Feb;42(2):23-31. PMID: 14908525.
- Kelechi TJ, Lukacs KS. Patient with dystrophic toenails, calluses, and heel fissures. J Wound Ostomy Continence Nurs. 1997 Jul;24(4):237-42. doi: 10.1016/s1071-5754(97)90121-2. PMID: 9274281.
- Swensson O, Langbein L, McMillan JR, Stevens HP, Leigh IM, McLean WH, et al. Specialized keratin expression pattern in human ridged skin as an adaptation to high physical stress. Br J Dermatol. 1998;139(5):767–75. doi: 10.1046/j.1365-2133.1998.02499.x
- Rubin L. Hyperkeratosis in response to mechanical irritation. J Invest Dermatol. 1949;13(6):313–5. doi: 10.1038/jid.1949.47
- Kim SH, Kim S, Choi HI, Choi YJ, Lee YS, Sohn KC, et al. Callus formation is associated with hyperproliferation and incomplete differentiation of keratinocytes, and increased expression of adhesion molecules. Br J Dermatol. 2010;163(3):495–501. doi: 10.1111/j.1365-2133.2010.09842.x
- Thomas SE, Dykes PJ, Marks R. Plantar hyperkeratosis: a study of callosities and normal plantar skin. J Invest Dermatol. 1985;85(5):394–7. doi: 10.1111/1523-1747.ep12277052
- Farndon L, Barnes A, Littlewood K, Harle J, Beecroft C, Burnside J, Wheeler T, Morris S, Walters SJ. Clinical audit of core podiatry treatment in the NHS. J Foot Ankle Res. 2009;2:7. doi: 10.1186/1757-1146-2-7. ]
- Alavi A, Sanjari M, Haghdoost A, Sibbald RG. Common foot examination features of 247 Iranian patients with diabetes. Int Wound J. 2009;6(2):117–22. doi: 10.1111/j.1742-481X.2009.00583.x.
- Benvenuti F, Ferrucci L, Guralnik JM, Gangemi S, Baroni A. Foot pain and disability in older persons: an epidemiologic survey. J Am Geriatr Soc. 1995;43(5):479–84. doi: 10.1111/j.1532-5415.1995.tb06092.x.
- Dunn JE, Link CL, Felson DT, Crincoli MG, Keysor JJ, et al. Prevalence of foot and ankle conditions in a multiethnic community sample of older adults. Am J Epidemiol. 2004;159(5):491–8. doi: 10.1093/aje/kwh071
- Harvey I, Frankel S, Marks R, Shalom D, Morgan M. Foot morbidity and exposure to chiropody: population based study. BMJ. 1997;315(7115):1054–5. doi: 10.1136/bmj.315.7115.1054
- Spink MJ, Menz HB, Lord SR. Distribution and correlates of plantar hyperkeratotic lesions in older people. J Foot Ankle Res. 2009;2:8. doi: 10.1186/1757-1146-2-8.
- Pataky Z, Golay A, Faravel L, Da Silva J, Makoundou V, Peter-Riesch B, et al. The impact of callosities on the magnitude and duration of plantar pressure in patients with diabetes mellitus. A callus may cause 18,600 kilograms of excess plantar pressure per day. Diabetes Metab. 2002;28(5):356–61.
- Murray HJ, Young MJ, Hollis S, Boulton AJ. The association between callus formation, high pressures and neuropathy in diabetic foot ulceration. Diabet Med. 1996;13(11):979–82. doi: 10.1002/(SICI)1096-9136(199611)13:11<979::AID-DIA267>3.0.CO;2-A
- Reiber GE, Vileikyte L, Boyko EJ, del Aguila M, Smith DG, Lavery LA, et al. Causal pathways for incident lower-extremity ulcers in patients with diabetes from two settings. Diabetes Care. 1999;22(1):157–62. doi: 10.2337/diacare.22.1.157.
- Menz HB, Lord SR. Foot pain impairs balance and functional ability in community-dwelling older people. J Am Podiatr Med Assoc. 2001;91(5):222–9. doi: 10.7547/87507315-91-5-222
- Mickle KJ, Munro B, Lord SR, Menz HB, Steele JR. Foot pain, plantar pressures, and falls in older people: a prospective study. J Am Geriatr Soc. 2010;58(10):1936–194. doi: 10.1111/j.1532-5415.2010.03061.x
- Del Rosso JQ, Levin J. Clinical relevance of maintaining the structural and functional integrity of the stratum corneum: why is it important to you? J Drugs Dermatol. 2011;10(10 Suppl):s5–12. [
- Bikowski J. Hyperkeratosis of the heels: treatment with salicylic acid in a novel delivery system. Skinmed. 2004;3(6):350–1. doi: 10.1111/j.1540-9740.2004.04056.x.
- Goldstein JA, Gurge RM. Treatment of hyperkeratosis with Kerafoam emollient foam (30 % urea) to assess effectiveness and safety within a clinical setting: a case study report. J Drugs Dermatol. 2008;7(2):159–62.
- Akdemir O, Bilkay U, Tiftikcioglu YO, Ozek C, Yan H, Zhang F, et al. New alternative in treatment of callus. J Dermatol. 2011;38(2):146–50. doi: 10.1111/j.1346-8138.2010.00978.x.
- Potts RO. Stratum corneum hydration: experimental techniques and interpretation of results. J Soc Cosmet Chem. 1986;37:9–33
- Barba C, Méndez S, Roddick-Lanzilotta A, Kelly R, Parra JL, Coderch L. Cosmetic effectiveness of topically applied hydrolysed keratin peptides and lipids derived from wool. Skin Res Technol. 2008;14(2):243–8. doi: 10.1111/j.1600-0846.2007.00280.x
- Ciampi E, van Ginkel M, McDonald PJ, Pitts S, Bonnist EY, Singleton S, et al. Dynamic in vivo mapping of model moisturiser ingress into human skin by GARfield MRI. NMR Biomed. 2011;24(2):135–44. doi: 10.1002/nbm.1562
- Springett K, Merriman L. Assessment of the Skin and its Appendages. In: Merrimen MM, Tollafield RT, editors. Assessment of the Lower Limb. London: Churchill Livingstone; 1995. p. 207
- Pham HT, Exelbert L, Segal-Owens AC, Veves A. A prospective, randomized, controlled double-blind study of a moisturizer for xerosis of the feet in patients with diabetes. Ostomy Wound Manage. 2002;48(5):30–6.
- Baumgart E. Stiffness–an unknown world of mechanical science? Injury. 2000;31 Suppl 2:S-B14–23.
- Hashmi F, Wright C, Nester C, Lam S. The reliability of non-invasive biophysical outcome measures for evaluating normal and hyperkeratotic foot skin. J Foot Ankle Res. 2015;8:28. doi: 10.1186/s13047-015-0083-8
- Clarys P, Clijsen R, Taeymans J, Barel AO. Hydration measurements of the stratum corneum: comparison between the capacitance method (digital version of the Corneometer CM 825®) and the impedance method (Skicon-200EX®) Skin Res Technol. 2012;18(3):316–23. doi: 10.1111/j.1600-0846.2011.00573.x.
- Sans N, Faruch M, Chiavassa-Gandois H, de Ribes CL, Paul C, Railhac JJ. High-resolution magnetic resonance imaging in study of the skin: normal patterns. Eur J Radiol. 2011;80(2):e176–81. doi: 10.1016/j.ejrad.2010.06.002.
- Neto P, Ferreira M, Bahia F, Costa P. Improvement of the methods for skin mechanical properties evaluation through correlation between different techniques and factor analysis. Skin Res Technol. 2013;19(4):405–16.
- Feldman DL. Which dressing for split thickness skin graft donor sites? Ann Plast Surg 1991, 27(3): 288-91
- Pavicic T, Korting HC. Xerosis and callus formation as a key to the diabetic foot syndrome: dermatological view of the problem and its management. J Dtsch Dermatol Ges 2006, 4(11): 935-41
- Ahanchian N, Nester C, Howard D, Ren L. 3D modelling of the human heel pad. Salford Postgraduate Annual Research Conference 2012, 31-36. Available at: usir.salford. ac.uk/29427/1/2012_proceedings_v2.pdf
- Hashmi F, Nester C, Wright C, Newton V, Lam S.
- Characterising the biophysical properties of normal and hyperkeratotic foot skin. J Foot Ankle Res 2015, 12(8): 35
- Dockery GL. Mechanical Injuries. In: Cutaneous Disorders of the Lower Extremity 1997. WB Saunders, Pennsylvania, p242
- Iversen MM, Midthjell K, Tell GS, et al. The association between history of diabetic foot ulcer, perceived health and psychological distress: the Nord-Trøndelag Health Study. BMC Endocr Disord 2009, 9:18. Available at: http://bmcendocrdisord.biomedcentral.com/ articles/10.1186/1472-6823-9-18
- Bristow I. Emollients in the care of the diabetic foot. Diabetic Foot J 2013, 16(2): 63-6
- Cork MJ, Danby S. Skin barrier breakdown: a renaissance in emollient therapy. Br J Nurs 2009, 18(14): 872-7
- Penzer R. Emollients: selection and application. Podiatry Now 2005, 9: S1-S8
- Springett K, Deane M, Dancaster P. Treatment of corns, calluses and heel fissures with a hydrocolloid dressing. J Br Podiatr Med 2001, 52(7): 102-4
- National Institute of Health and Care Excellence. Type-2 Diabetes: Prevention and management of foot problems. Clinical guideline 10, January 2004. NICE, London. Available at: www.nice.org.uk/guidance/ cg10?unlid=93368616920162723333
- Young M, Townson M, Hicks G. A photographic scale to aid appropriate foot skin care for people with diabetes. Diabetic Foot J 2014, 7(2): 70
- Draelos ZD. Eczema Regimens. In: Draelos ZD (Ed), Cosmetic Dermatology: Products and Procedures, 2nd edn. John Wiley & Sons Ltd, Oxford, 2015
- Steel C, Longhurst B. An appraisal of IMUderm [Unpublished data]
- Beam JW. Tissue adhesives for simple traumatic lacerations. J Athl Train 2008, 43(2): 222–4
- Feldman DL. Which dressing for splitthickness skin graft donor sites? Ann Plast Surg 1991, 27(3): 288-91 17.
- Mertz PM, Davis SC, Cazzaniga AL, Drosou A, Eaglstein WH. Barrier and antibacterial properties of 2-octyl cyanoacrylate-derived wound treatment films. J Cutan Med Surg 2003, 7(1): 1-6
- Coulthard P, Esposito M, Worthington HV, van der Elst M, van Waes OJF, Darcey J. Tissue adhesives for closure of surgical incisions. Cochrane Database Syst Rev 2010, 12(5): CD004287
- Longhurst B, Allan E, Bristow IR. The use of cyanoacrylates in the management of dry heel fissures: a preliminary study. Podiatry Now 2010, 13(9): 11-15
- Vlahovic TC, Hinton EA, Chakravarthy D, Fleck CA. A review of cyanoacrylate liquid skin protectant and its efficacy on pedal fissures. J Am Col Certif Wound Spec 2011, 2(4): 79-85
read this next

At The Foot Hub clinics we offer a new painless fungal nail treatment: Photodynamic Antimicrobial Therapy (PACT® )

At The Foot Hub we run through all treatment options to our patients and recommend treatment based on patient expectations, preferences, in line with evidence based medicine.