Fungal Toenail
What is a fungal toenail and how do you get rid of it?
What are the treatment options and how effective are they?
It is estimated that 10% of Australians have an active fungal toenail infection, making it one of the more common condition we see in our foot clinics. Fungal toenail infection constitutes approximately 50% of all toenail conditions. An active infection can be moderately contagious but thankfully risk of transmission to loved ones can be reduced when the condition is managed correctly. With proper assessment, diagnosis and an individually tailored treatment plan even the most severe cases can be resolved.
At our foot clinics in Sydney patients can select from a comprehensive range of treatment options. When attending the clinic for the first time our honest and empathetic staff will discuss with you the various treatment modalities; their benefits, cost, success rates and potential side effects. If required in-house testing can also be performed to confirm diagnosis of fungal toenail infection on the spot. In some case your Podiatrist may also have to consult with your family GP to arrange prescription of oral antifungal medication.
Fungal toenail infections as notoriously difficult to resolve but after you see one of our Podiatrists you can rest easy knowing each treatment plan is geared specifically to your needs to achieve the best outcome.
what is a fungal toenail?
A fungal toenail infection or onychomycosis is where a fungal organism enters and infects the toenail complex. It can be caused by different types of fungal organisms but the most common is Trichophyton rubrum present in over 90% of all cases. Other dermatophytes can cause fungal toenail infections Trichophyton interdigitale, Trichophyton mentagrophytes or Tichophyton tonsuran). Yeasts (candida species) and nondermatophyte moulds can also cause fungal toenail infections.
These are the four main types of a fungal toenail infection:
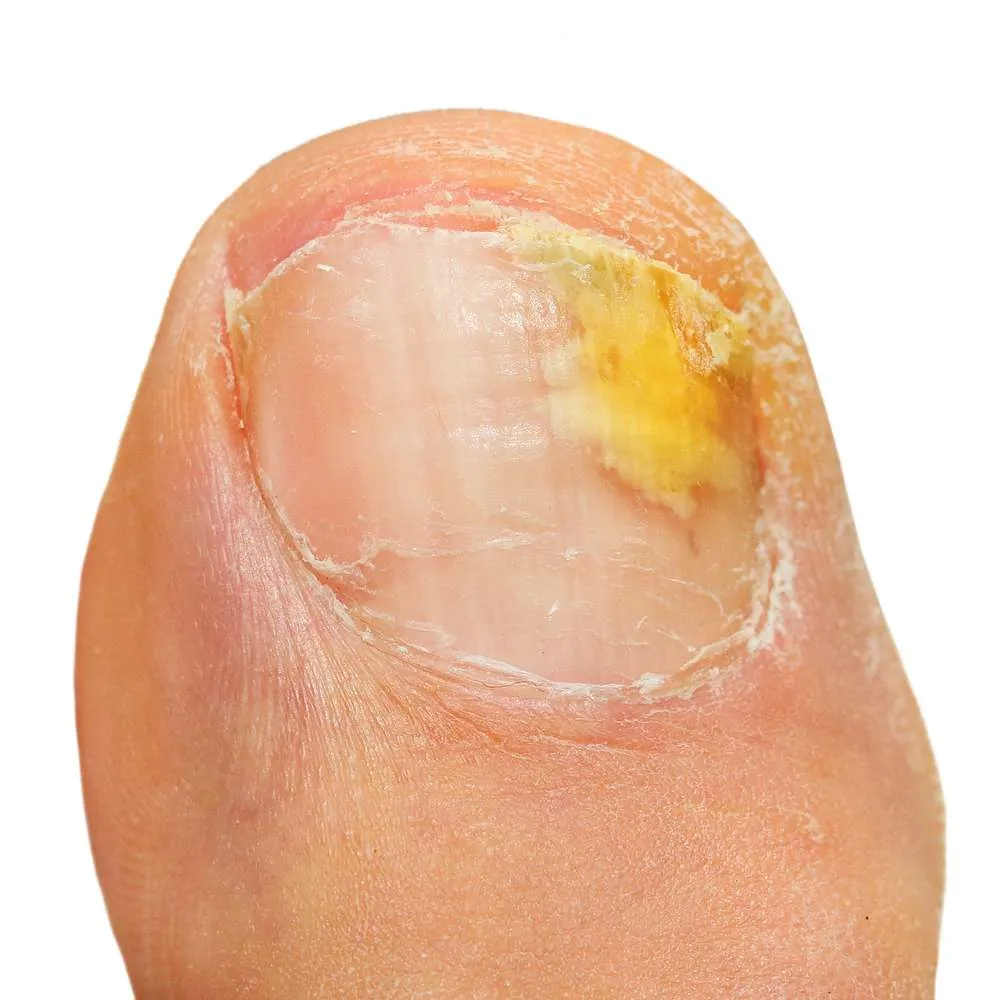
Distal lateral subungual onychomycosis (DLSO)
This is a fungal toenail infection always caused by dermatophyte infection. It infects the lateral edges initially and then spreads down to the nail bed. There is usually tinea pedis/athlete’s foot found in the skin around the toenail.
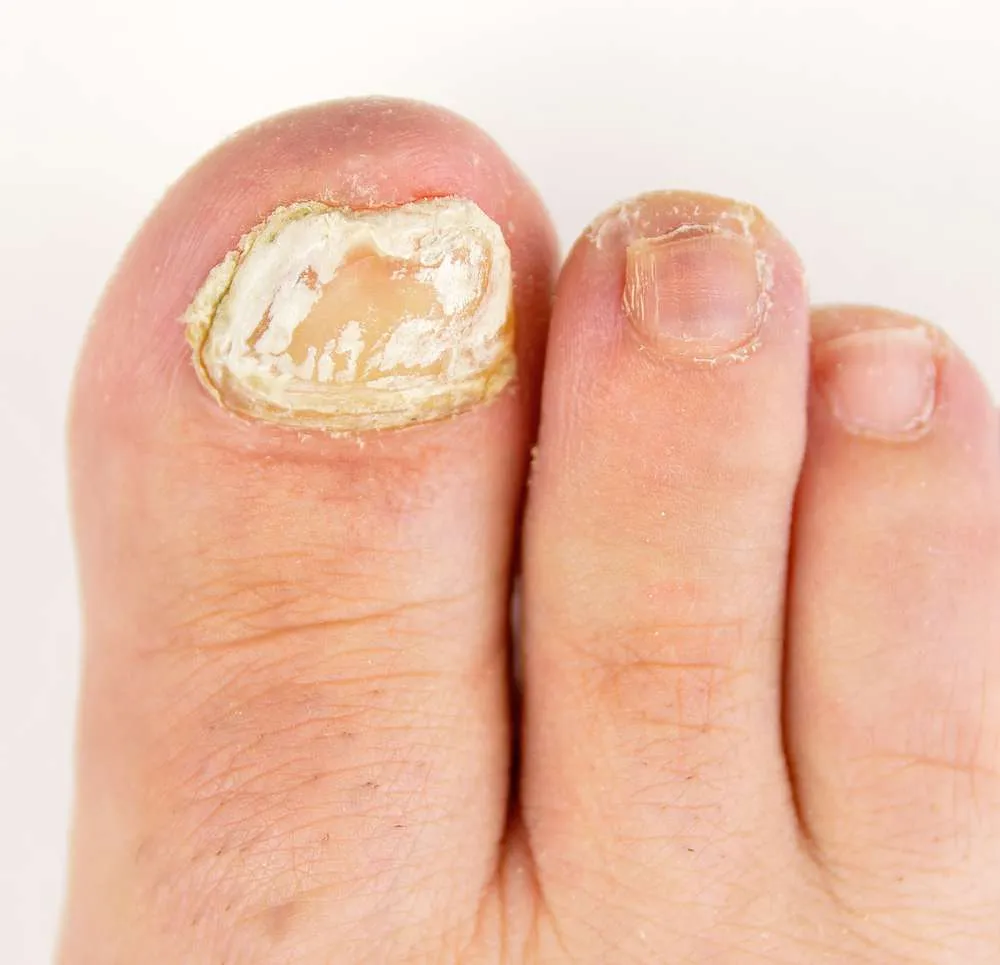
Superficial white onychomycosis (SWO)
This type of fungal toenail infection is commonly caused by Trichophyton mentagrophytes affecting the surface of the nail plate rather than the nail bed; and is white in discoloration and nail plate is noticeably flaky.

Proximal white sub-ungual onychomycosis (PWSO)
This is an uncommon fungal toenail infection caused by rare strain of dermatophyte (Trichophyton tonsurans, Trichophyton mentagrophytes, Epidermophyton floccosum) often related to intercurrent disease among immunosuppressed patients. This is commonly seen in people with vascular disease and diabetes
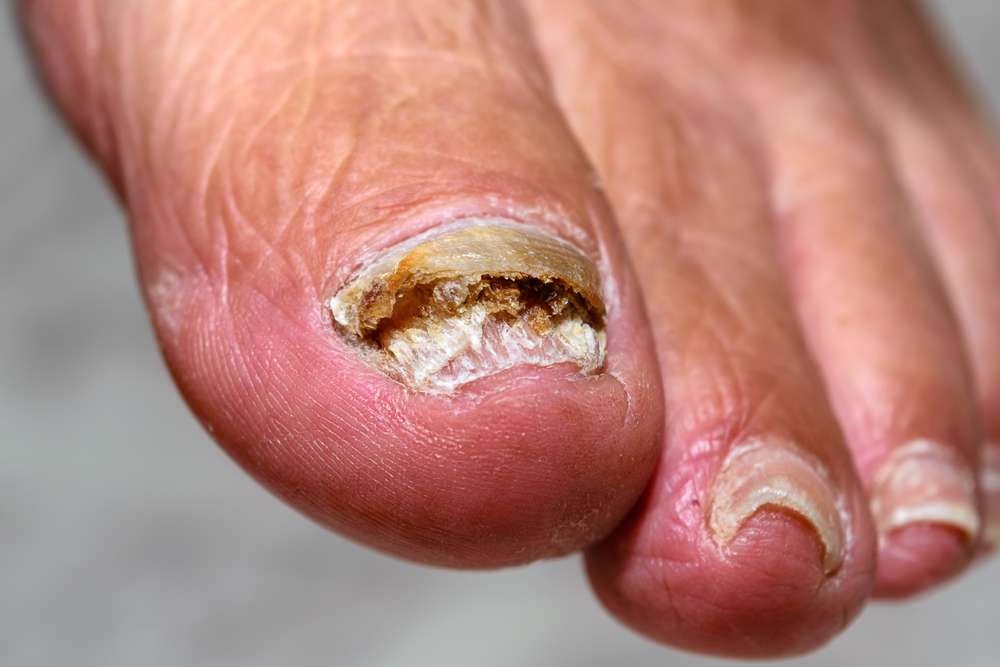
Total dystrophic onychomycosis (TDO)
This is where the infection progresses, and the entire nail plate is completely contaminated and damaged.
Signs of a fungal toenail infection
Fungal toenail infections can be mistaken for other nail conditions as there are similarities in the physical presentation. Here are a few of the signs and symptoms of fungal toenail infection:
- Yellow, brown, or white discoloration of the nail plate
- Nail deformation
- Nail thickening
- Nail lifting
- Presence of powdery white patches
- Presence of nail pits
- Excessive keratin/ nail protein deposits

How do you get a fungal toenail infection?
- Minor skin or nail injuries
- Nail deformities or disease
- Prolonged exposure to moist conditions
- Using nail clippers that have been used on other people
- Wearing closed-in-footwear that is not breathable
risk factors for fungal toenail infections
There are a few accepted factors which can increase your chance of developing a fungal toenail infection:

Advanced age

cross infection at home

Sporting activities

Diabetes

Genetic predisposition

Immunodefiency

Nail trauma

Peripheral vascular disease

Psoriasis

Smoking

frequent immersion in water

Athletes foot
testing for fungal toenails
It’s important to make sure that you have the correct diagnosis when it comes to fungal toenails. Properly identification is not only essential in treatment but also for prevention. Testing can occur in the form of microscopy and culture. Your GP can send you for both these tests after taking toenail clippings however it’s important to know that:
- Microscopy can be negative 20% of cases
- Culture can give a false negative in 40% of cases
At the Foot Hub we offer a quick five-minute test which can gives accurate and clear result (98% success rate) for fungal toenails. Toenail clippings are taken during your appointment and tested looking for the presence or absence of dermatophytes in under 5 minutes by having a simple colour change. This allows us to accurately diagnosis fungal toenail infections where there is doubt and proceed with treatment.
Quality of life
Fungal toenail infection, like other foot conditions, is treatable and manageable. We understand that a fungal toenail infection and can affect your day to day life causing feelings of embarrassment and anxiety.
The embarrassment and anxiety caused by having the fungal toenail infection can adversely affect your social, emotional, and psychological well-being. As a result, some of our patients avoid activities such as swimming, going to the beach or wearing open shoes. A fungal toenail is not a life-threatening condition and there are numerous treatments available and we are here to help by providing treatment solutions to help your feel better about your feet and toenails.
podiatrist assessment
Despite the high prevalence of fungal toenail infections and accounting for 50% of nail disorders, not all toenail discolouration is a fungal toenail. Podiatrists can assess and help diagnosis your toenail condition accurately. There are other toenail conditions that can look like a fungal toenail infection, these include:
- Psoriasis
- Toenail trauma
- Thickened toenails due to ageing
- Other conditions such as melanoma
Your Podiatrist will assess your toenail, medical history and take into account treatments which you may have tried in the past and provide an individualised fungal toenail treatment plan for you.

fungal toenail treatment
There are numerous ways to treat a fungal toenails infection. Effectiveness of treatment depends on how severe the infection is, type, symptoms, and any underlying medical conditions. At The Foot Hub we run through all treatment options to our patients and recommend treatment based on patient expectations, preferences, in line with evidence based medicine. The first stage to treatment is always patient education. We believe that understanding what a fungal toenail infection and its causes can help you understand this condition better and thus lead to better clinical outcomes.
Treatment expectations
Fungal toenails are very challenging to treat. We understand that fungal toenail infections can be unsightly, and many people would like their toenail to revert to “normal. The goal of treatment is to eradicate the infection, restore the toenail and prevent reinfection. In some cases, if the infection has been there for a long period of time, your toenail may not return to “normal” as permanent damage maybe have occurred. It's important to have realistic expectations regarding treatment. Make sure to discuss with your Podiatrist if you have any concerns.
There is no quick treatment for fungal toenail infections, treatment can range from 6-24 months. This is due to the slow growing nature of toenails which are further impacted by an active fungal toenail infection.
Whilst we understand what causes fungal toenail infections there is no 100% proven treatment. Throughout your treatment journey, your Podiatrist may change or modify your treatment if needed.
Treatment options
Nail filing
Before treatment commences, we recommend anyone with a fungal toenail have a general podiatry treatment where the affected toenails are trimmed, and nail plate is filed down by a podiatry drill.
Toenails need to be 2mm thick for most antifungal toenail therapy to work, this also means home treatments like lacquers. There needs to adequate penetration into the nail plate and if your toenail is thick there is a low chance treatment (topicals, laser or medication) will work effectively.

Topical anti-fungals
Topical antifungals tend to be the initial treatment for most people with fungal toenail infections. This is usually an over the counter nail lacquer that is either purchased or compounded in a pharmacy. Treatment works by filing down the toenail and applying a liquid to the nail plate either daily or weekly depending on package instructions. There are many brands available and results vary amongst many people. To ensure a higher success rate we recommend:
- Filing down your toenail to allow penetration before each application. If your toenail is severely thickened before starting application book an appointment for toenail filing. This will allow the medication to enter your nail plate and destroy the fungal organism
- Apply the treatment not only the discoloured spot but the entire toenail plate and also 5mm of the surrounding skin. Studies have shown higher success rates.
- Be patient. Look out for new clear growth, a healthy toenail grows 1.7mm a month. It may be slower with an infected toenail.

Oral Medication
Due to the limited efficacy of topical antifungals, oral medication can be recommended for treatment. The mostly commonly used drug is Terbinafine (oral Lamisil) which has a cure rate of 70%-80%, making it the most effective fungal toenail treatment. Other medications include Itraconazole or fluconazole.
Treatment duration depends on severity of infection and can take up to 12-24 weeks. Oral Lamisil is approved for safe use in Australia through prescription and is available on the Pharmaceutical Benefit Scheme. Like all medications, Terbinafine can cause side effects, but not everyone gets it them and will go way when you stop taking it. There are common side effects which 1 in 100 can experience and severe side effects being rare. We recommend talking to your GP for more information and eligibility for medication.

In some cases, you may not want to or be able take or oral medication and have unsuccessfully tried topical antifungal treatment, PACT therapy can be a good treatment option. PACT therapy is a LED treatment that uses a photosensitising gel that causes fungal cell destruction. It is different to laser therapy which works by inhibiting growth of fungal cells. At our foot clinics we offer PACT therapy as an effective treatment option for our patients.

In cases of total dystrophic onychomycosis where the entire toenail plate has been affected, chemical nail avulsion maybe warranted. In the past doctors would recommend surgical removing the toenail and commencing treatment. This is unnecessary as simply using a 40% cream on a toenail for a few weeks can bring about a painless way of removing a thickened and damaged toenail before starting antifungal treatment.

Home Remedies
There are some natural remedies containing anti-fungal and anti-bacterial properties which you can use at home:
- Tea tree oil
- Apple cider vinegar

Research has shown that when treatments are used in combination there is a higher success rate. At The Foot Hub you fungal treatment plan maybe combinational to help achieve better clinical outcomes
prevention
Prevention is the number one solution to combat fungal toenail infections. Here are some of the ways for you to prevent and the stop a fungal toenail from occurring:
- Avoid walking barefoot in public spaces e.g. showers, locker rooms, gyms
- Change your foot socks and shoes regularly
- Keep nails short and straight across
- Use an antifungal spray or powder in your shoes
- Wear open shoes to aerate your toes and feet
- Hot wash your socks and if possible, with an antifungal wash
- Make sure to dry your feet after a shower
- If you wear steel cap boots for work, make sure they are well ventilated

complications of fungal toenails
Fungal toenail infection is treatable and manageable and strict observance of care plan should successfully treat the infection. There are instances; however, where fungal toenail treatment becomes difficult and persistent due to the following reasons:
- Reoccurrence
- Nail lifting
- Spreading
- Infecting others around you
frequently asked questions
There is no quick treatment to fungal toenail infection. Treatment would depend on the severity of the condition and your treatment preferences.
Fungal toenails are moderately contagious. They can be transmitted from one human to another especially among household with family members infected with fungus on toenail.
Anybody can get infected with fungal toenail infection. However there are some people who are more susceptible than others.
You may have more risk factors for developing fungal infections. It’s important to know that once you have had a fungal toenail infection, there is a chance of reoccurrence.
No, you should not ignore your fungal toenail infection as it can worsen if left untreated leading to more serious condition such as permanent nail damage, infection in other toenails and tinea pedis
Consult with your podiatrist if you suspect you have fungal toenail infection for earlier treatment plan.
Unfortunately, fungal toenail infection, like other infections, does not go away on its own. Consult with your podiatrist for any type of foot concerns for treatment options and correct professional diagnosis of your foot condition.
- Bristow IR. The effectiveness of lasers in the treatment of onychomycosis: a systematic review. J Foot Ankle Res. 2014;7:34.
- Carney C, Tosti A, Daniel R, Scher R, Rich P, DeCoster J, et al. A new classification system for grading the severity of onychomycosis: Onychomycosis Severity Index. Arch Dermatol. 2011;147(11):1277-82.
- Crawford F, Ferrari J. Fungal toenail infections. Clin Evid. 2006(15):2212-20.
- Elewski BE. Onychomycosis: pathogenesis, diagnosis, and management. Clin Microbiol Rev. 1998;11(3):415-29.
- Elewski BE. Once-weekly fluconazole in the treatment of onychomycosis: introduction. J Am Acad Dermatol. 1998;38(6 Pt 2):S73-6.
- Elewski BE. Onychomycosis: pathogenesis, diagnosis, and management. Clin Microbiol Rev. 1998;11(3):415-29.
- Gupta AK, Stec N, Summerbell RC, Shear NH, Piguet V, Tosti A, et al. Onychomycosis: a review. J Eur Acad Dermatol Venereol. 2020.
- Hanna S, Andriessen A, Beecker J, Gilbert M, Goldstein E, Kalia S, et al. Clinical Insights About Onychomycosis and Its Treatment: A Consensus. J Drugs Dermatol. 2018;17(3):253-62.
- Jansen R, Redekop WK, Rutten FF. Cost effectiveness of continuous terbinafine compared with intermittent itraconazole in the treatment of dermatophyte toenail onychomycosis: an analysis of based on results from the L.I.ON. study. Lamisil versus Itraconazole in Onychomycosis. Pharmacoeconomics. 2001;19(4):401-10.
- Kreijkamp-Kaspers S, Hawke K, Guo L, Kerin G, Bell-Syer SE, Magin P, et al. Oral antifungal medication for toenail onychomycosis. Cochrane Database Syst Rev. 2017;7:CD010031.
- Lahfa M, Bulai-Livideanu C, Baran R, Ortonne JP, Richert B, Tosti A, et al. Efficacy, safety and tolerability of an optimized avulsion technique with onyster(R) (40% urea ointment with plastic dressing) ointment compared to bifonazole-urea ointment for removal of the clinically infected nail in toenail onychomycosis: a randomized evaluator-blinded controlled study. Dermatology. 2013;226(1):5-12.
- Lahfa M, Bulai-Livideanu C, Baran R, Ortonne JP, Richert B, Tosti A, et al. Efficacy, safety and tolerability of an optimized avulsion technique with onyster(R) (40% urea ointment with plastic dressing) ointment compared to bifonazole-urea ointment for removal of the clinically infected nail in toenail onychomycosis: a randomized evaluator-blinded controlled study. Dermatology. 2013;226(1):5-12.
- Lukasik P, van Asch M, Guo H, Ferrari J, Godfray HC. Unrelated facultative endosymbionts protect aphids against a fungal pathogen. Ecol Lett. 2013;16(2):214-8.
- Parker J. Management of common fungal infections in primary care. Nurs Stand. 2009;23(43):42-6.
- Piraccini BM, Balestri R, Starace M, Rech G. Nail digital dermoscopy (onychoscopy) in the diagnosis of onychomycosis. J Eur Acad Dermatol Venereol. 2013;27(4):509-13.
- Piraccini BM, Bruni F, Alessandrini A, Starace M. Evaluation of efficacy and tolerability of four weeks bifonazole treatment after nail ablation with 40% urea in mild to moderate distal subungual onychomycosis. G Ital Dermatol Venereol. 2016;151(1):32-6.
- Piraccini BM, Iorizzo M, Lencastre A, Nenoff P, Rigopoulos D. Ciclopirox Hydroxypropyl Chitosan (HPCH) Nail Lacquer: A Review of Its Use in Onychomycosis. Dermatol Ther (Heidelb). 2020.
- Piraccini BM, Rech G, Tosti A. Photodynamic therapy of onychomycosis caused by Trichophyton rubrum. J Am Acad Dermatol. 2008;59(5 Suppl):S75-6.
- Piraccini BM, Sisti A, Tosti A. Long-term follow-up of toenail onychomycosis caused by dermatophytes after successful treatment with systemic antifungal agents. J Am Acad Dermatol. 2010;62(3):411-4.
- Renner R, Grusser K, Sticherling M. 1,064-nm diode laser therapy of onychomycosis: results of a prospective open treatment of 82 toenails. Dermatology. 2015;230(2):128-34.
- Rich P, Scher RK, Breneman D, Savin RC, Feingold DS, Konnikov N, et al. Pharmacokinetics of three doses of once-weekly fluconazole (150, 300, and 450 mg) in distal subungual onychomycosis of the toenail. J Am Acad Dermatol. 1998;38(6 Pt 2):S103-9.
- Rigopoulos D, Papanagiotou V, Daniel R, 3rd, Piraccini BM. Onychomycosis in patients with nail psoriasis: a point to point discussion. Mycoses. 2017;60(1):6-10.
- Roberts DT, Taylor WD, Boyle J, British Association of D. Guidelines for treatment of onychomycosis. Br J Dermatol. 2003;148(3):402-10.
- Rodgers P, Bassler M. Treating onychomycosis. Am Fam Physician. 2001;63(4):663-72, 77-8.
- Savin RC, Drake L, Babel D, Stewart DM, Rich P, Ling MR, et al. Pharmacokinetics of three once-weekly dosages of fluconazole (150, 300, or 450 mg) in distal subungual onychomycosis of the fingernail. J Am Acad Dermatol. 1998;38(6 Pt 2):S110-6.
- Scher RK, Breneman D, Rich P, Savin RC, Feingold DS, Konnikov N, et al. Once-weekly fluconazole (150, 300, or 450 mg) in the treatment of distal subungual onychomycosis of the toenail. J Am Acad Dermatol. 1998;38(6 Pt 2):S77-86.
- Skelton J, Jusino MA, Li Y, Bateman C, Thai PH, Wu C, et al. Detecting Symbioses in Complex Communities: the Fungal Symbionts of Bark and Ambrosia Beetles Within Asian Pines. Microb Ecol. 2018;76(3):839-50.
- Stewart CR, Algu L, Kamran R, Leveille CF, Abid K, Rae C, et al. Impact of Onychomycosis and Treatment on Patient Reported Quality of Life Outcomes: A Systematic Review. J Am Acad Dermatol. 2020.
- Wang Y, Geizhals S, Lipner SR. Retrospective Analysis of Laboratory Abnormalities in Patients Prescribed Terbinafine for Onychomycosis. J Am Acad Dermatol. 2020.
- Wang Y, Geizhals S, Lipner SR. Trends in onychomycosis prescribing: a single center retrospective study over 15 years. J Dermatolog Treat. 2020:1-2.
- Westerberg DP, Voyack MJ. Onychomycosis: Current trends in diagnosis and treatment. Am Fam Physician. 2013;88(11):762-70.
- Wu AG, Geizhals S, Lipner SR. Retrospective Study of Factors Affecting Medication Adherence in Patients Prescribed Efinaconazole 10% Solution for Onychomycosis. J Am Acad Dermatol. 2020.
- Yang EJ, Lipner SR. Differences in price trends between branded and generic medications for onychomycosis. Dermatol Ther. 2020:e13928.
- Zalacain A, Merlos A, Planell E, Cantadori EG, Vinuesa T, Vinas M. Clinical laser treatment of toenail onychomycoses. Lasers Med Sci. 2018;33(4):927-33.
read this next

At The Foot Hub clinics we offer a new painless fungal nail treatment: Photodynamic Antimicrobial Therapy (PACT® )

Not all nail conditions are fungal toenails. It’s important to make sure that you have the correct diagnosis when treating your toenails as it can help improve treatment outcomes. Learn about other conditions that can effect your toenails.
